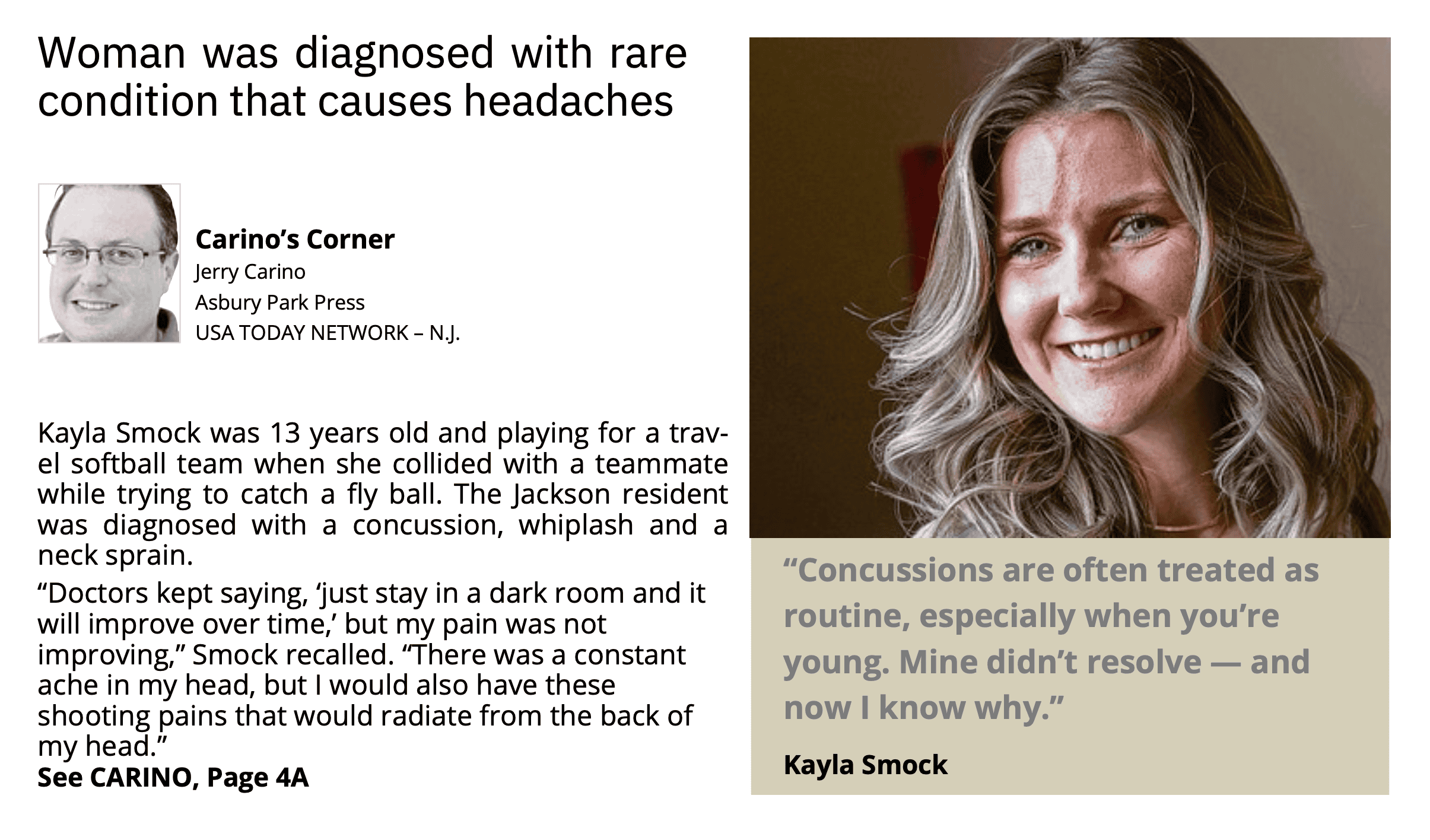Welcome!
My goal is to raise awareness, provide support and offer resources for those affected with Occipital Neuralgia in Canada.
What is Occipital Neuralgia?
Occipital neuralgia (ON) is a headache disorder caused by irritation, inflammation, or compression of the occipital nerves, which supply sensation to the back of the scalp. In simple terms, it’s nerve pain coming from the back of the head and neck, not a typical migraine or tension headache.
ON is also often misdiagnosed as cervicogenic headaches and sometimes even cluster headaches. People often, but not always describe occipital neuralgia as sharp, electric, stabbing, or shock-like pain that shoots upward from the base of the skull.
Sometimes the pain can feel pressure-like or throbbing in nature. People often say that their pain shoots upward toward the crown or eye, report burning or aching between attacks. Many times people also experience scalp tenderness or sensitivity to touch (even brushing hair hurts) or pain with pressure at the base of the skull. Sometimes light sensitivity or nausea (which can mimic migraine) also occur.
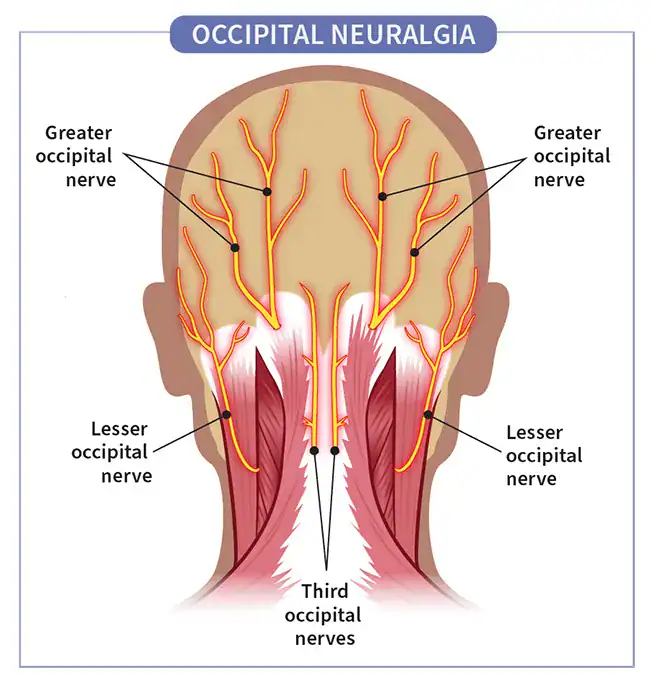
Three nerves are usually involved:
- Greater occipital nerve (C2) – most commonly
- Lesser occipital nerve (C2–C3)
- Third occipital nerve (C3)
These nerves travel from the upper cervical spine, through tight neck muscles and then into the scalp. Because they pass through muscle and fascia, these nerves can become compressed or irritated, which triggers neuropathic pain. Common causes include:
- Chronic neck muscle tightness/spasm
- Nerve entrapment in fascia or muscle
- Cervical spine arthritis or disc disease
- Prior head/neck trauma or whiplash
- Posture-related strain
- Scar tissue from surgery
- Less commonly: masses, cysts, or vascular compression
Remember the underlying problem is mechanical compression resulting in nerve hypersensitivity. The diagnosis is mainly clinical and based primarily on three items: A consistent history, physical exam, and a good response to nerve blocks. Imaging is typically unhelpful except to rule out other causes such as brain tumors, aneurysms, etc. It is reasonable to try conservative treatment modalities first such as physical therapy, massage, acupuncture, and sometimes certain medications (e.g. Botox). However, surgical intervention has been shown to be incredibly effective and very safe in appropriately selected patients and in experienced hands.
Resources
"This foundation was built to create the community and resources I wish had existed before and during my diagnosis.Together we are making the invisible visible."
- Kayla Smock, President & Founder of ONF
"Occipital neuralgia isn’t just a headache it's a peripheral nerve problem. Every nerve has a story, be it compressed, inflamed, or injured, and we can change that story. When you treat the nerve(s), you treat the pain, so my job isn’t to manage the pain. It’s to find the nerve(s) causing it and fix the problem at its source. Living with constant head pain isn’t normal and it isn’t something you just have to accept. Relief is possible. Restoration is real."
- Dr. Ziv Peled, MD
Plastic Surgeon & Peripheral Nerve Specialist
More Resources
-
How & Why Did I Get Occiptal Neuralgia
The title of this post is often the million dollar question. I have posted many times in the past about how ON can be caused by compression from spastic neck muscles, compression by tight connective tissue (i.e., fascia) and/or compression from surrounding blood vessels. Many of the patients I see have had headaches ever since…
-
Migraine or Neuralgia – Which do I have?
People often confuse migraine symptoms with something called neuralgia. The former refers to an often disabling neurological condition characterized by severe and sometimes frequent headaches. The latter literally means “nerve pain” with the implication that the condition in question is secondary to some type of nerve injury or dysfunction. While migraines can be sub-classified in…
-
Decompression vs. Excision for Injured Nerves
One of the most important intraoperative decisions a peripheral nerve surgeon must make is whether an injured nerve should be decompressed or transected. These terms are sometimes used interchangeably with “excision,” but that is not technically correct. Excision implies complete removal of a structure—such as a tumor or cyst. Peripheral nerves, however, are not removed…
-
The MRI Was Negative. Now What?!?
Like many things in medicine—and in life—a result can be viewed from more than one perspective. A “negative” or “normal” MRI does not mean that nothing is wrong. It simply means that certain serious conditions were not found. And that’s an important place to start. On the positive side, your scan might show: These are…
New Jersey Newspaper Article from November 2025. Click to open full article PDF.